
Keep Your Dog Safe From Rattlesnake Bites
 By Barry Neichin, DVM
By Barry Neichin, DVM
Pawsitive Teams’ Director of Veterinary Medicine
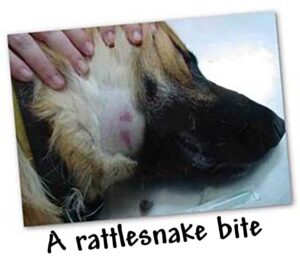
It’s a beautiful weekend in San Diego. A typical summer day. I’ve been at work all day and hoping to leave work as scheduled and catch some sun by the pool this afternoon. Just as I am about to leave work, the front desk calls back and says Mrs. Smith is on her way in with Clifford. Clifford is a 100-pound golden retriever that has limitless energy—he’s one of my favorite patients. He’s rushed to the back of the hospital. He’s lying on his side, his gums are pale, and his pulse is weak. His face is swollen to the size of a basketball. There are two small puncture wounds on the left side of his face and there are a few drops of blood dripping onto the exam table. The underside of his lip is bruised, and poor Clifford can barely raise his head.
 Mrs. Smith explained to the nurse that Clifford was hiking with them on the trails in Escondido. Suddenly, he was barking at a rattlesnake and then ran away whimpering. Immediately his face began to swell. Mr. Smith knew that Clifford had been bitten by the rattlesnake and immediately carried him the two miles back to their car. He knew to keep Clifford calm and minimize his activity along the way. They had lost one of their previous Golden Retrievers, Goldie, to a snakebite, so they knew the drill and knew that ABC Veterinary Hospital had antivenin to help Clifford.
Mrs. Smith explained to the nurse that Clifford was hiking with them on the trails in Escondido. Suddenly, he was barking at a rattlesnake and then ran away whimpering. Immediately his face began to swell. Mr. Smith knew that Clifford had been bitten by the rattlesnake and immediately carried him the two miles back to their car. He knew to keep Clifford calm and minimize his activity along the way. They had lost one of their previous Golden Retrievers, Goldie, to a snakebite, so they knew the drill and knew that ABC Veterinary Hospital had antivenin to help Clifford.
We placed an IV, drew blood to access his clotting time, complete blood count, and chemistries. Fluids were started immediately, along with antibiotics to prevent infection and antihistamines. The antivenin was already prepared, and we immediately started the infusion and careful monitoring to make sure Clifford’s vital signs improved and that he didn’t have an allergic reaction to the medicine. He would spend the night under observation. While Clifford was being treated, I reviewed essential information about snake bites.
 Rattlesnake bites are frequently seen in practice in Southern California, with about 150,000 bites occurring annually. Many backyards are located near canyons that are natural habitats for a few different rattlesnakes species. Dogs are twenty times more likely than people to be bitten by venomous snakes. Snakebites are very painful, life-threatening, and expensive to treat. Dogs are often curious or protective when they encounter a snake and most bites involve their face or front extremities. The toxins in a snakebite can cause severe local swelling, pain, and systemic toxicity. The toxins can be dangerous to the heart, nerves, liver and cause generalized bleeding problems and shock. Some dogs can die suddenly, and others are minimally affected. The severity of the bite varies depending on a variety of factors including the size of the snake, the age of the snake, when the snake ate last, and importantly the species of the snake. While the Western Diamondback Rattlesnake is the most common snake in this area, Southern California is also home to the
Rattlesnake bites are frequently seen in practice in Southern California, with about 150,000 bites occurring annually. Many backyards are located near canyons that are natural habitats for a few different rattlesnakes species. Dogs are twenty times more likely than people to be bitten by venomous snakes. Snakebites are very painful, life-threatening, and expensive to treat. Dogs are often curious or protective when they encounter a snake and most bites involve their face or front extremities. The toxins in a snakebite can cause severe local swelling, pain, and systemic toxicity. The toxins can be dangerous to the heart, nerves, liver and cause generalized bleeding problems and shock. Some dogs can die suddenly, and others are minimally affected. The severity of the bite varies depending on a variety of factors including the size of the snake, the age of the snake, when the snake ate last, and importantly the species of the snake. While the Western Diamondback Rattlesnake is the most common snake in this area, Southern California is also home to the  Southern Pacific Rattlesnake, whose bites can be even more dangerous. The Rattlesnake vaccine (by Red Rock Biologics) was developed with Western Rattlesnake inactivated venom, but the manufacturer has found cross protection with other species of snakes.
Southern Pacific Rattlesnake, whose bites can be even more dangerous. The Rattlesnake vaccine (by Red Rock Biologics) was developed with Western Rattlesnake inactivated venom, but the manufacturer has found cross protection with other species of snakes.
The best way to keep your pet safe is by avoiding a bite in the first place. Staying on trails and keeping your pet on a leash are extremely helpful. If your yard is adjacent to snake habitat, using critter fencing to keep snakes out can be an important first step to preventing an encounter. Even with careful avoidance, some snake encounters cannot be avoided. And with avoidance training, your dog can be trained to stay away from snakes. This training is offered by experts who have access to “safe” snakes and the use of a shock collar to train the dog to stay away. I’ve heard the training can be harsh but for most dogs it is highly effective and may save their life.
Another protective tool available to us is a licensed vaccine by Red Rock Biologics. The vaccine is given prior to rattlesnake season. I usually recommend starting the vaccine series in February. The first time your pet is vaccinated, your pet will receive two doses. The following year, we’ll begin semi-annual to annual boosters. The effectiveness of the vaccine is controversial. Original studies on mice showed improved survivability, decreased swelling and pain which looked convincing. In practice, it’s difficult to assess because bites vary so much in severity. The goal of vaccination is to produce antibodies to the venom that is injected by the bite of a snake. The antibodies neutralize the toxins in the venom so that the pet experiences less pain and swelling and reduces the risk of mortality. However, several retrospective studies analyzing outcomes of snake bites in dogs who have been bitten have called the efficacy of the vaccine into question. The most common adverse reaction is a sterile abscess or swelling at the site of injection which may need treatment. In my professional experience, such reactions are rare, occurring in about 1 out of every 100 dogs that are vaccinated. Because the efficacy is still in question and the vaccine may have side effects, I limit vaccination to dogs at high risk.
If you’ve seen snakes in your yard, or if your dog hikes with you, I certainly recommend vaccination. However, if your pet is indoors and is unlikely to be exposed, the rattlesnake vaccination may not be appropriate for your pet. One important reminder is that even if your dog is vaccinated, your pet will require veterinary care. The vaccine is designed to decrease the severity of the reaction, improve survivability, and buy you more time to seek care, but it doesn’t eliminate the need for treatment.
If a rattlesnake bites your pet, you should take your pet to the veterinarian immediately. Make sure you know where your pet can receive antivenin. Not all veterinary clinics stock antivenin, so plan ahead and check with your veterinarian to see if they are prepared to manage your emergency before you need their service.
Later that night, Clifford looked much better and wagged his tail when I kneeled next to him to check his vitals. He bounced up and licked my face and I knew he was on the road to recovery. Although I missed the sunny afternoon, I slept well that night knowing Clifford was going to go home tomorrow. If you think your pet is at high risk for a snake bite and would like to discuss your pets’ specific needs, please email me at [email protected]



